Structural Empowerment
Clinical nurses have a voice within the UT Southwestern shared governance organizational structure, built on a solid foundation of teamwork and collaboration. Shared decision-making and accountability empower nurses with a process for determining professional nursing practice. These organizational standards are developed through staff-led interdisciplinary committees, task forces, and councils to improve patient outcomes and experiences. Nurses at all levels take conscious ownership of patient care, safety, ethics, research, performance improvement, and evidence-based practice. Our shared governance structure supports the practicing nurse as a key decision-maker with a credible, sought-after perspective. This model strengthens practice by supporting relationships and partnerships among clinical areas, providing an innovative and collaborative environment that bolsters our quality patient outcomes.
UTSW Shared Governance Structure
At UT Southwestern Medical Center, Shared Governance was formally refreshed and relaunched this past year to better reflect the evolving work of councils across the organization. The revised model was intentionally designed to represent ongoing interdisciplinary collaboration and to strengthen decision-making authority at all levels of practice. The updated framework reinforces a culture in which clinical nurses, advanced practice providers, leaders, and interprofessional partners actively contribute to practice standards, quality initiatives, and strategic priorities. UTSW maintains a robust Shared Governance structure that engages staff from all areas and disciplines, promoting transparency, accountability, and shared decision-making, as reflected in the following diagram.
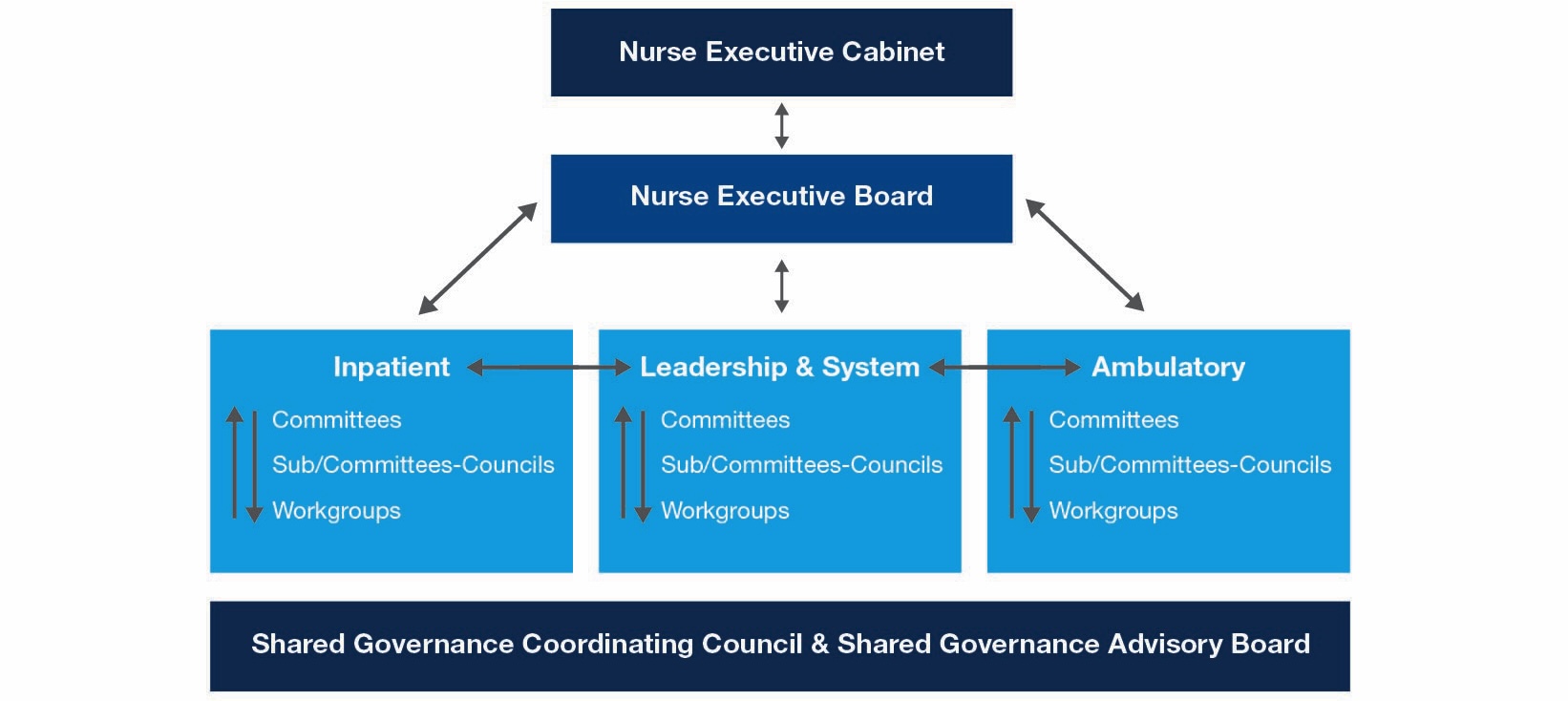
This model illustrates the three-tier decision-making structure that empowers nurses to influence clinical practice, policy, and improvement initiatives across the health system. It begins with unit-based councils (UBCs), where frontline nurses identify and address local practice needs. Recommendations escalate to specialty and strategic councils for broader coordination and expert review. The Shared Governance Coordinating Council (SGCC) ensures alignment, prioritization, and systemwide communication. The Nursing Executive Board provides strategic integration, and the Nurse Executive Cabinet (NEC) serves as the highest nursing authority, ensuring decisions align with organizational priorities and nursing excellence.

Specialty Certifications and Education Levels
UT Southwestern nurses validate their mastery of skills, knowledge, and abilities through certification and meet ongoing learning and practice requirements through recertification. The certification process assures patients and their families that the nurse caring for them has demonstrated experience, knowledge, and skill in the complex specialty of their care. Nursing certification and continuing education contribute to an environment of professionalism and a culture of retention. Certification also differentiates UT Southwestern from other health care organizations, demonstrating to consumers that we have attracted the most skilled and experienced nursing professionals. By the end of calendar year 2025, UTSW employed 2,712 specialty certified nurses.

With 79.3% of our nurses holding a B.S.N. or higher, our team has nearly reached the elite 80% national benchmark established by the Institute of Medicine. This achievement is particularly significant because it places UTSW nurses well ahead of the national average, which current data from the National Council of State Boards of Nursing (NCSBN) and the American Association of Colleges of Nursing (AACN) places at approximately 71.7% to 73%. By maintaining this exceptionally high standard of education, our nurses demonstrate a superior commitment to clinical excellence and advanced patient care that outpaces most health care systems across the country.
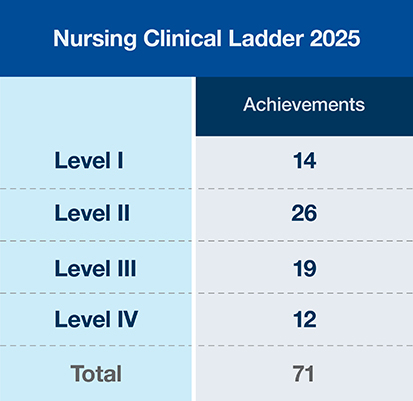
Clinical Ladder
The UT Southwestern Nursing Clinical Ladder program is committed to recognizing superior performance and rewarding nursing excellence in providing direct patient care. The newly improved program offers a unified, point-tiered system for all eligible nursing staff throughout UT Southwestern. Within the program, participants may select options unique to their individual professional development and nursing practice in areas of continuing education, quality improvement, leadership, and evidence-based practice.
The UTSW Clinical Ladder is open to all clinical nurses involved in direct patient care.

Empowering Growth: Elevating RNs through the Clinical Ladder Journey
This initiative was implemented in Unit 6G to promote professional growth and engagement among registered nurses (RNs) by advancing them on the Clinical Ladder (CL). Leadership identified the need for improvement after recognizing that no nurses were participating in the CL program. The primary goal of this project was to increase RN participation and awareness of the CL process, fostering a culture of professional development and recognition. Baseline data included 49 eligible RNs, with a target of 25% participation by the end of the project. This initiative aimed to enhance nursing excellence, motivation, and retention by supporting nurses in achieving higher levels of clinical practice and leadership.
Assistant Nurse Manager Julie Abraham led implementation of the new CL program on Unit 6G as part of a professional development initiative. After collaborating with the hospital’s Clinical Ladder Committee to understand the program framework, she introduced the process and communicated details via email to all staff, with reminders via Quick Hits and staff meetings. Julie conducted one-on-one meetings with eligible nurses to discuss program benefits, assist with letters of intent, and guide them through the selection of required activities, including committee involvement, unit-based projects, precepting, and participation in grand rounds. She provided continuous follow-up and support to ensure successful completion and submission of applications.
The implementation of the CL initiative on Unit 6G resulted in meaningful improvements in professional development and staff engagement, making nurses feel recognized and appreciated for their growth. Prior to the intervention, there were no Unit 6G participants in the CL program. Following Julie’s focused efforts, 15 of 49 eligible RNs (31%) successfully advanced on the CL, surpassing the initial goal of 25%. This achievement reflects a strengthened culture of professional accountability and growth. Nurses became more involved in unit-based projects, committees, precepting, and educational opportunities, demonstrating increased ownership of their practice and alignment with the Magnet model of excellence.
Contributors:
- Julie Abraham, B.S.N., RN
- Sahri Ann Dino Vu, M.S.N., RN, CCRN, NE-BC
- Beena Johnson, M.S.N., RN, RN-BC
Advanced Practice Provider Incentive Program
In fiscal year 2023, the Advanced Practice Provider (APP) Clinical Ladder program was replaced with the APP Incentive Program, which incorporated operational goals in the quality and productivity domains, while keeping the professional contribution goals that were paramount to the Clinical Ladder program’s success. The APP Incentive Program was developed with feedback from APPs and key organizational stakeholders. The professional contribution domain provides an opportunity to receive an incentive from activities such as:
- Involvement in quality improvement, evidence-based practice, and research projects
- Serving as a podium speaker or presenting a poster abstract at a conference
- Publishing in a scholarly journal or book
- Supporting UTSW’s educational mission through precepting and/or teaching
- Serving on UTSW, partner organization, or professional organization committees
In FY 2025, 319 advanced practice registered nurses received an incentive payment for their professional contributions to the organization and our profession. This value represents 44% of eligible APRNs at UTSW.
Supporting APP Employees Who Seek Doctoral Education
Beginning in June 2023, the Office of Advanced Practice Providers (OAPP) APP Student Office implemented a structured process to support APP employees pursuing doctoral education and to ensure alignment with UT Southwestern compliance and IRB requirements. From June through August 2023, standardized tools were developed, including a decision-making tree to determine appropriate affiliation agreements, a REDCap intake survey, resource guides, and a standardized presentation. The process has since identified 29 APP employees planning or enrolled in doctoral programs, including 21 Doctor of Nursing Practice, three Doctor of Medical Science, two Doctor of Philosophy, two Doctor of Nurse Anesthesia Practice, and one Doctor of Science in Physician Assistant Studies programs. The process was communicated through APP forums, newsletters, and leadership channels to support early engagement.
Since implementation, the APP Student Office and the Program Manager for Research and Academic Partnerships have supported APP employees by securing required affiliation agreements, redesigning projects when needed, facilitating networking, and serving as system preceptors to support timely project completion. As of fiscal year 2026, 13 APP employees have graduated, 12 are currently enrolled, two are implementing doctoral projects, and two are pending affiliation agreements for spring 2026. In addition, three APP employees received the Rory Meyers Education Program for Nursing Excellence Advanced Degree Scholarship for fiscal year 2026. Overall, this initiative has strengthened doctoral preparation, scholarly engagement, and professional growth within the APP workforce.
Contributors:
- Rubria Marines-Prices, D.N.P., Ph.D., APRN, ACNP-BC
- Christopher Roe, D.N.P., APRN, ACNP-BC
- Ebony C. Glenn
APP Mentorship Committee
The APP Mentorship Committee has been active since 2016, and in FY2025 it enrolled its largest cohort to date. The APP Mentorship Program is a yearlong formal professional development program in which a mentee is paired one on one with a mentor to address a specific, measurable, achievable, relevant, and time-bound (SMART) goal defined by the mentee. APPs apply and are matched according to their desired goal and the mentor’s relevant experience. The committee is spearheaded by a mentorship committee comprising staff APPs and an OAPP executive sponsor. In FY2025, the committee was chaired by Anitha Litty, D.N.P., APRN, AGACNP-BC, FNP-C CDCES; Ashley Boothe, M.S., APRN, AGACNP-BC, served as Chair-Elect. The executive sponsor of the committee was Briana Whitherspoon, D.N.P., M.B.A., APRN, ACNP-BC. Fifteen mentees successfully completed the program, each paired with an APP mentor.
The APP Mentorship Program demonstrated a strong and positive impact over the year, as reflected in participant survey results. Approximately 80% of respondents either “strongly agreed” or “somewhat agreed” that, after completing the mentorship program, they “felt more satisfied with their jobs,” and equally, 80% reported “feeling more socially connected at work.” When asked whether they felt more certain about their overall professional goal after completing the program, 90% of the participants either “strongly agreed” or “agreed.” Perceptions of program quality were similarly positive, with about half rating the program “good” and roughly 40% as “excellent.” Overall, about 90% of the participants reported that the mentoring program was useful, underscoring its value as a key initiative for employee satisfaction, connection, and professional development. The mentorship committee is looking forward to contributing to the ongoing professional development of APPs and keeping them engaged to our organization’s tripartite mission.
Hospital and Ambulatory Clinical Education and Professional Development
The Departments of Clinical Education and Professional Development (CEPD) for hospital and ambulatory staff advance the philosophy, mission, and vision of UTSW Nursing Services. CEPD provides support to clinical staff by offering education, training, and professional development activities. This includes clinical orientation, student placement, and education on care standards and quality improvement. Our practice transition team supports and facilitates the transition to practice experience while cultivating an inclusive learning environment for our RN and PCT residents and nurse fellows. We are accredited as a provider of nursing continuing professional development by the American Nurses Credentialing Center's Commission on Accreditation. We offer educational hours for events that support nursing continuing professional development (NCPD) and improve patient outcomes. CEPD is committed to providing clinical staff with education and resources to deliver safe, compassionate, patient-centered care in an engaging learning environment of quality, evidence-based, and professional practice.
Our commitment to excellence in education is evidenced by employing the Nursing Professional Development Practice Model (ANPD, 2016) to leverage learning to meet and exceed organizational outcomes. To meet this challenge, our Nursing Professional Development (NPD) practitioners are master’s degree level-prepared nurses and require NPD certification within 18 months of hire. The NPD practitioners operationalize environmental scanning, proactively plan educational programming, and work collaboratively with unit-based educators to meet the learning needs at the individual, unit/clinic, and organization levels.
In 2025, we welcomed the following cohorts:
- Cohort 16 – 62 residents, 26 fellows
- Cohort 17 – 81 residents, 24 fellows
- Cohort 18 – 56 residents, 38 fellows







